Value of Arthroscopic Knee Surgery ‘Inconsequential’
/By Pat Anson, Editor
Arthroscopic knee surgery on older adults has become a routine procedure in North America and Europe – with over 850,000 arthroscopies performed every year to relieve knee pain in the UK and the United States alone.
But a new study published in the The BMJ questions the evidence behind the procedure and calls the benefit of knee surgery “inconsequential.” The article is part of The BMJ's “Too Much Medicine” campaign, which highlights the waste of resources and potential harm caused by unnecessary medical care.
“The small inconsequential benefit seen from interventions that include arthroscopy for the degenerative knee is limited in time and absent at one to two years after surgery,” the report says. “Taken together, these findings do not support the practice of arthroscopic surgery for middle aged or older patients with knee pain with or without signs of osteoarthritis.”
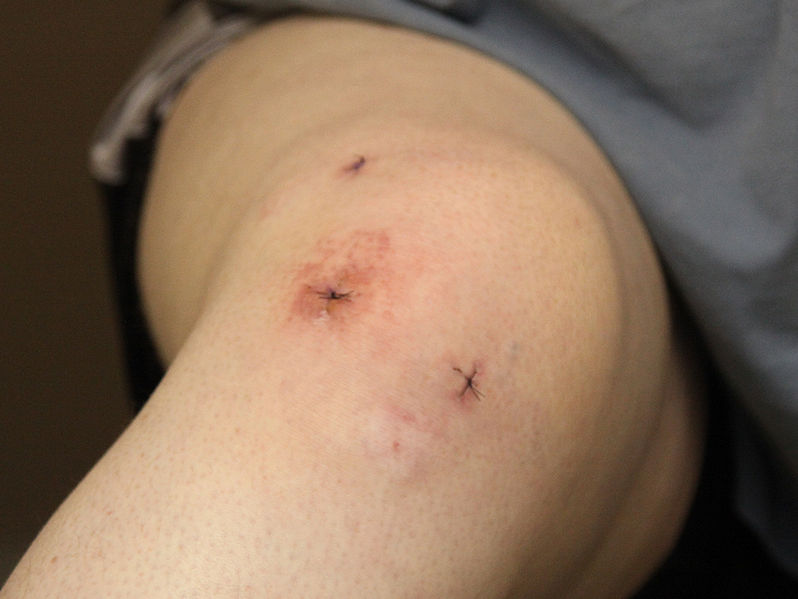
Knee arthroscopies are a type of “keyhole” surgery in which the surgeon makes a small incision in the knee and inserts a tiny camera and instruments to diagnose and repair damaged ligaments or torn meniscus. Many specialists are convinced of the benefits of the surgery.
But when researchers in Denmark and Sweden reviewed 18 studies on arthroscopic knee surgery, they found that half were of poor quality or lacked a placebo control. The other nine studies found that the surgery provided pain relief for up to six months, but without any significant benefit in physical function.
Risks associated with arthroscopic knee surgery, although rare, include deep vein thrombosis (DVT), infection, pulmonary embolism, and death.
"It is difficult to support or justify a procedure with the potential for serious harm, even if it is rare, when that procedure offers patients no more benefit than placebo," argues Professor Andy Carr from Oxford University’s Institute of Musculoskeletal Sciences in an accompanying editorial.
With rates of knee surgery at their current level, Carr says thousands of lives could be saved and DVTs prevented each year if the procedure was discontinued or diminished.
“We may be close to a tipping point where the weight of evidence against arthroscopic knee surgery for pain is enough to overcome concerns about the quality of the studies, confirmation bias, and vested interests. When that point is reached, we should anticipate a swift reversal of established practice,” Carr wrote.
The BMJ study is not the first to question the value of arthroscopic knee surgery. A 2014 report by a German health organization found the procedure provides no benefit to patients with osteoarthritis, and does not relieve pain any better than physical therapy or over-the-counter pain medications.
Another large study in Australia also questions the value of arthroscopic knee surgery, finding there was no significant benefit for osteoarthritis patients.
The American Medical Society for Sports Medicine (AMSSM) lists arthroscopic knee surgery as one of five procedures that are not always necessary in the Choosing Wisely campaign. The AMSSM advises physicians to avoid recommending knee arthroscopy as a treatment for patients with degenerative meniscal tears.
Depending on insurance, hospital charges and the surgeon, arthroscopic knee surgery costs about $4,000.