Why Doctors Don’t Do What Works
/By Barby Ingle, Columnist
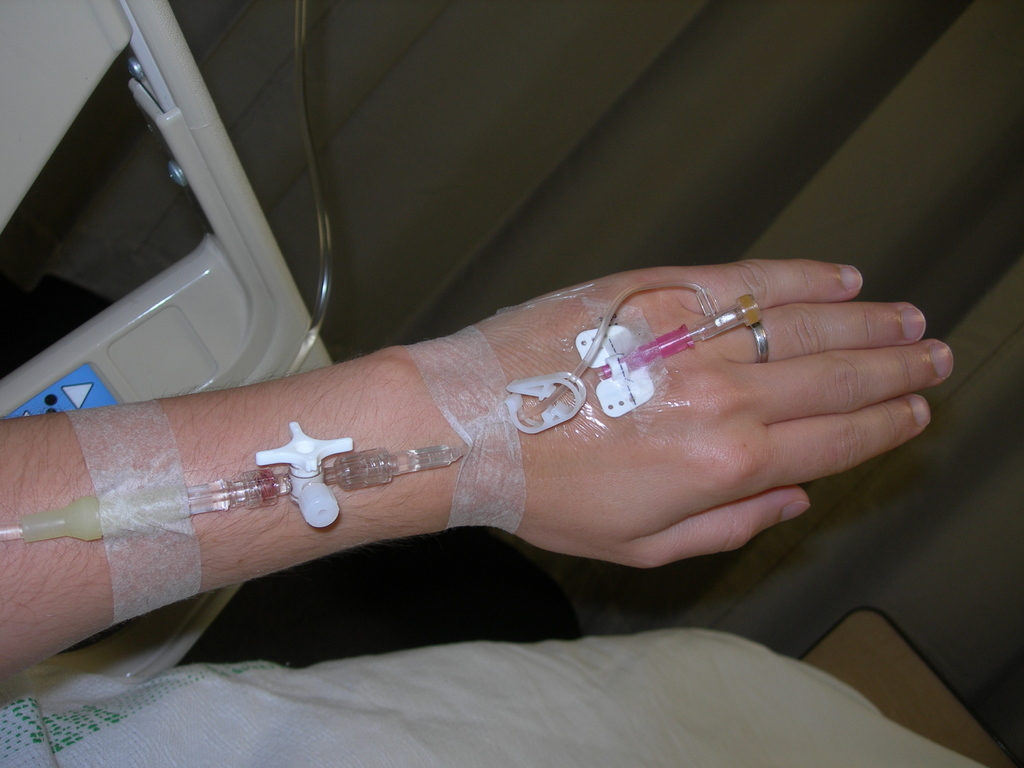
Let’s examine infusion therapies. There are multiple types, including intravenous ketamine, plasma, stem cell, immunoglobulin and lidocaine.
I have tried many of these and know from personal experience that they can work. I have also been by the side of friends who have undergone infusions with great success, including some who have gone into remission.
Infusion therapy is being performed for patients with all kinds of neuropathy conditions and it helps many recipients. It is just hard to find a doctor who will perform infusions for anything outside of IV-chemotherapy for cancer patients. Why?
Right off the bat, let’s consider costs. In the case of intravenous immunoglobulin, it is very expensive to make, so insurance companies fight it a lot and that discourages doctors from offering it.
IV-lidocaine offers some relief, but is short lasting. In the case of IV-ketamine, it is an inexpensive drug and insurance companies are covering it in many cases, depending on documentation and the protocol being used.
I know that many doctors are underpaid. They are getting cutback by insurance companies and on treatment reimbursements with Medicare. Malpractice insurance rates are very high and many doctors still have thousands of dollars in student loans to pay. Those that have their own practice make less because of the overhead costs of location and staffing.
As a former business owner, I see the valid points the doctors are making. As a patient, I wish I could fix these reasons so that more patients could be helped.
Since learning about IV therapies myself back in 2007, I started asking around for names of doctors who are performing them as viable treatment option for chronic pain diseases. What I found was that the list was very small. I started asking questions of pain doctors specifically. I did not do this as “patient Barby,” but as director of the International Pain Foundation.
Some of these doctors have seen me over the past 10 years go from “wheels to heels.” They cannot believe their eyes when they see me now. Yet they still give reasons and obstacles for not wanting to offer infusion treatments.
Many have very small offices. Even at pain management and surgical facilities, the patient takes up a spot in the recovery room or infusion room for half a day. That becomes prohibitive for doctors to deal with because it cuts down the number of patients they can treat and the amount of money they can make.
In medical school, doctors have to choose a specialty. They get general studies that include a little info on this and a little on that, but unless a doctor is interested in studying the specialty that includes your condition, they may not have ever heard of it. Even if they did study your particular condition, they may have gotten only four hours of training on it.
Looking at it from the other side, doctors do have little time for treating patients, and they have required continuing education hours that they also have to fit in. Some tend to stick to classes that reflect their area of interest, so they are not getting a wide variety of knowledge that, as patients, we tend to believe occurs. I learned the hard way that doctors are not created equal. If an illness or condition is not their specialty, they do not invest in it.
When you have an IV-ketamine infusion, a certified nurse needs to be present and monitor you the entire time. He or she can’t just come and go. Taking one staff member away for four hours at a time increases a doctor’s overhead expenses. Most doctors could not survive this type of set up. They need to see more patients.
Not only are you taking vital staff away when getting an IV infusion, you are using space. If you are taking up a chair in the recovery room at a doctor’s facility for hours, the doctor is unable to fill that chair with other paying patients. Not just paying patients, but patients who also need help, just as much as you do.
When insurance companies start to compensate doctors appropriately for IV therapies, it will resolve many of these issues and more doctors will offer infusions. I pray that it becomes widespread as an option.
In 2007, I was at a medical conference where Dr. Robert Schwartzman was speaking on infusion therapy and he said, “It will soon be the standard treatment for RSD patients.”
“Soon” in medical terms can often be 8 to 10 years. It is about time that we get better access to proper and timely care.
Barby Ingle suffers from Reflex Sympathetic Dystrophy (RSD) and endometriosis. Barby is a chronic pain educator, patient advocate, and president of the International Pain Foundation. She is also a motivational speaker and best-selling author on pain topics.
More information about Barby can be found at her website.
The information in this column should not be considered as professional medical advice, diagnosis or treatment. It is for informational purposes only and represents the author’s opinions alone. It does not inherently express or reflect the views, opinions and/or positions of Pain News Network.