Can Oxygen Therapy Treat Fibromyalgia?
/By Pat Anson, Editor
Hyperbaric oxygen therapy – also known as HBOT – has been used for decades to treat infections, severe burns, carbon monoxide poisoning, even scuba divers recovering from decompression sickness.
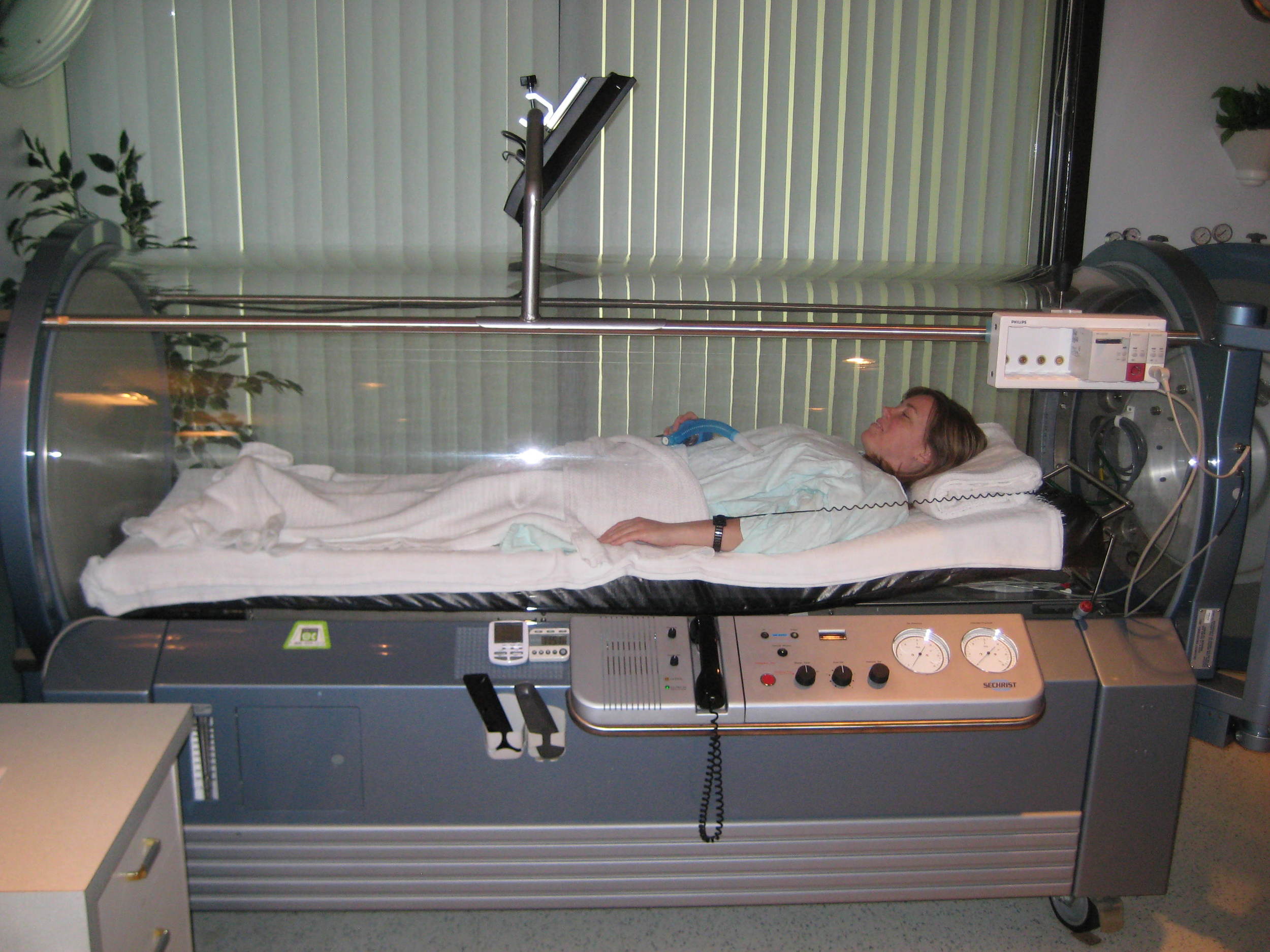
Patients undergoing HBOT are put in a pressurized room or tube. The higher air pressure allows lungs to gather more oxygen than they would normally – helping the body to heal faster.
Promising new research out of Israel suggests that HBOT can also be used to treat fibromyalgia patients by causing neuroplasticity – a “re-wiring” of the brain that can change neural activity in areas overly sensitized by chronic pain. The study has been published in the journal PLoS ONE.
“This study provides evidence that HBOT can improve quality of life and well-being of many FMS (fibromyalgia) patients. It shows for the first time that HBOT can induce neuroplasticity and significantly rectify brain activity in pain related areas of FMS patients,” wrote lead author Shai Afrati, MD, of the Institute of Hyperbaric Medicine, Assaf Harofeh Medical Center.
file photo of a woman getting hyperbaric oxygen therapy
Fibromyalgia is a poorly understood disorder that is characterized by deep tissue pain, headaches, fatigue, depression and insomnia. The cause is unknown and there is no cure.
Afrati, who has also studied oxygen therapy on stroke and concussion victims, enrolled 60 female fibromyalgia patients in his latest study. For five days each week they were given 90 minutes of HBOT with oxygen enriched air.
“It is plausible that increasing oxygen concentration by HBOT can change the brain metabolism and glial function to rectify the FMS-associated brain abnormal activity. It has already been demonstrated that exposure to hyperbaric oxygen induces significant anti-inflammatory effect in different conditions and pathologies,” said Afrati.
After two months, brain imaging showed the women had significant changes in neural activity, and they reported less pain and fewer tender points. Several said that they had either reduced or stopped taking pain medication.
However, not everyone could handle being placed in a pressurized air chamber. Five women dropped out of the study, complaining of dizziness, claustrophobia and an inability to adjust to the air pressure.
But Afrati is encouraged by the results.
“Follow-up studies are needed in order to investigate the durability of the HBOT effects on FMS. It might be that some patients will need more HBOT sessions,” he wrote. “Since there is currently no solution for FMS patients, and since HBOT is obviously leading to significant improvement, it seems reasonable to let FMS patients benefit from HBOT, if possible, now rather than wait until future studies are completed.”