Critics Question Oxygen Therapy for Fibromyalgia
/By Pat Anson, Editor
Some experts are challenging the findings of a new clinical study that found that hyperbaric oxygen therapy (HBOT) could be used to treat -- and possibly even cure -- fibromyalgia.
Israeli researchers gave HBOT therapy to dozens of women suffering from fibromyalgia and found there was a significant improvement in their pain and other symptoms. The women were put in pressurized air chambers and breathed pure oxygen for 90 minutes, five times a week for two months.
Researchers say brain scans of the women before and after HBOT proved their theory that additional oxygen alters brain pathology and "repairs" parts of the brain overly sensitized by chronic pain.
"Brain pathology? This is speculation being presented as established knowledge," said John Quintner, MD, an Australian rheumatologist who maintains that fibromyalgia is not a disease, but a "symptom cluster" that could have many different causes.
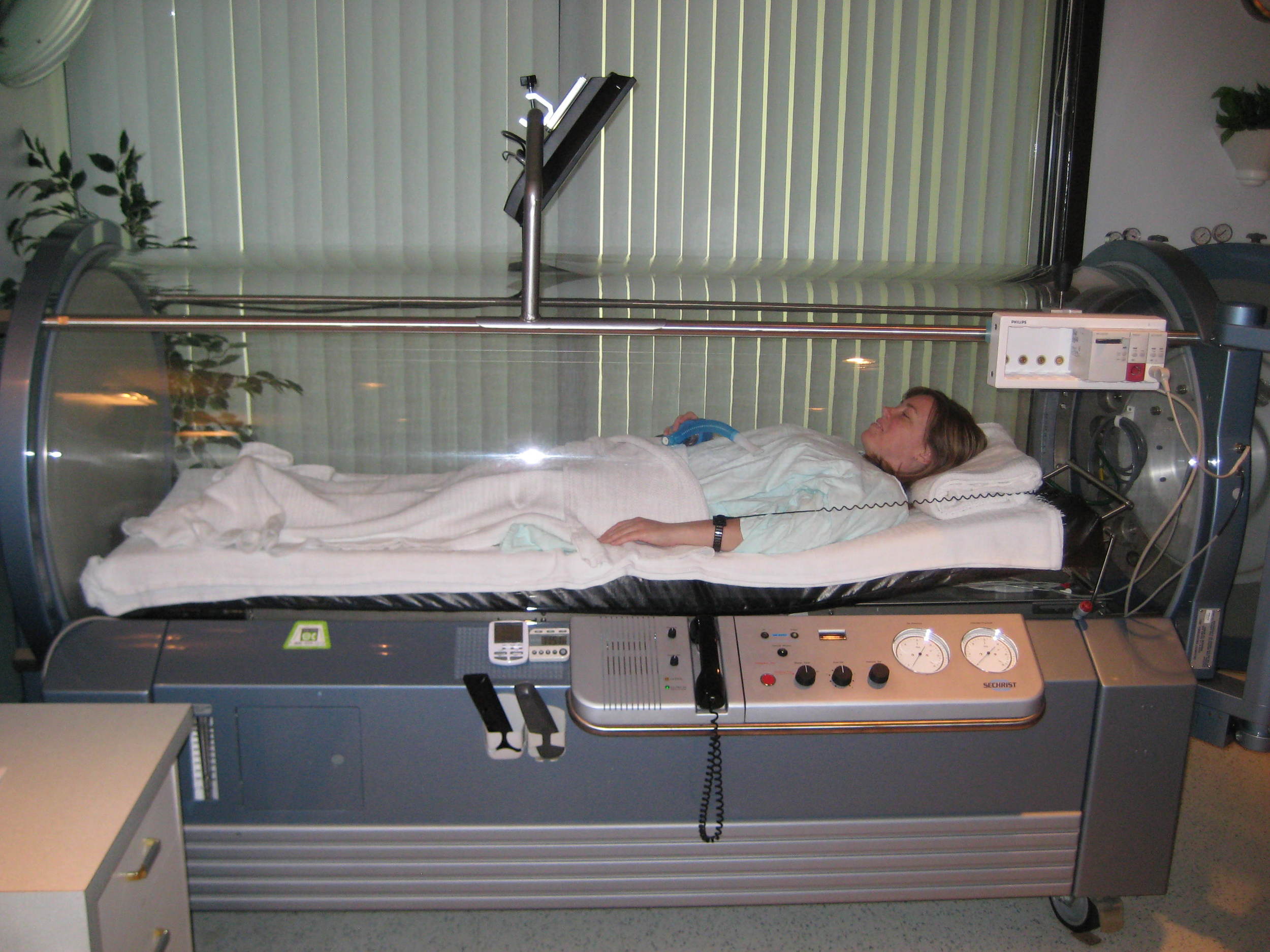
tHE INTERIOR OF A HYPERBARIC CHAMBER. COURTESY OF Sagol Center for Hyperbaric Medicine and Research
Fibromyalgia is a poorly understood disorder that is characterized by deep tissue pain, headaches, fatigue, depression and insomnia. The cause is unknown.
"This clinical trial is using a methodology that is predicated upon fibromyalgia being a distinct medical condition," said Quintner, telling Pain News Network that the study proved little, but was "good news for those who manufacture portable HBOT units."
Researchers at the Sagol Center for Hyperbaric Medicine and Research at the Assaf Harofeh Medical Center and Tel Aviv University were studying the use of HBOT on stroke and concussion patients when they realized that oxygen therapy might also change the neural activity of patients with fibromyalgia.
"Patients who had fibromyalgia in addition to their post-concussion symptoms had complete resolution of the symptoms," said Shai Efrati, MD, lead author of the study that is published online in PLoS ONE.
Efrati said some patients will require follow-up sessions of HBOT and some won't need to.
"We have learned, for example, that when fibromyalgia is triggered by traumatic brain injury, we can expect complete resolution without any need for further treatment. However, when the trigger is attributed to other causes, such as fever-related diseases, patients will probably need periodic maintenance therapy."
HBOT puts more oxygen into the bloodstream, which delivers it to the brain. Efrati's earlier studies found that HBOT induces neuroplasticity, which leads to repair of chronically impaired brain functions. Most of the women who participated in the new study had fibromyalgia that the researchers believe was triggered by brain trauma.
DR. SHAI EFRATI
"Symptoms in about 70 percent of the women who took part have to do with the interpretation of pain in their brains," said Eshel Ben-Jacob, a study co-author who is an adjunct professor of biosciences at Rice University. "They're the ones who showed the most improvement with hyperbaric oxygen treatment. We found significant changes in their brain activity.
"Most people have never heard of fibromyalgia. And many who have, including some medical doctors, don't admit that this is a real disorder. I learned from my MD friends that this is not the only case in which disorders that target mainly women raise skepticism in the medical community as to whether they're real or not."
HBOT Claims Called "Crazy"
One of those skeptics is Fred Wolfe, MD, a prominent fibromyalgia researcher who says the Israeli study lacks proper controls used in most clinical studies -- such as patients being "blinded" to whether they are receiving treatment or a placebo.
"The fibromyalgia study world is filed with positive studies based on unacceptable controls," said Wolfe. "While I don't know enough about this treatment to be sure, I would tend to think the symptomatic improvement could be based on control and blinding problems. It is possible that the demonstrated effect on the brain of oxygen is separate from the effect of symptoms."
Wolfe is particularly troubled by a recommendation at the end of the study that fibromyalgia patients should undergo HBOT therapy now, "rather than wait until future studies are completed.”
"I could only characterize (that) as crazy. Crazy because of the money it would cost and crazy because it posits fibromyalgia as brain disease. FM is not a disease and there is a difference between mechanism and causes. One needs some replication before jumping in," said Wolfe in an email to Pain News Network.
Many fibromyalgia patients are ready to jump in, based on the comments from readers to our first report about the Israeli study.
"Where do you find studies like this to volunteer? I would so do this," wrote one fibromyalgia sufferer.
"I would so try this. I often feel like I'm not getting enough oxygen," said another.
"Sign me up, please," a woman wrote.
"Is this available in Tucson or Phoenix, Arizona?" asked another woman.
Many fibromyalgia sufferers are desperate for any kind of treatment that would provide relief, much less a cure. In the Israeli study, several patients either drastically reduced or eliminated their use of pain medications.
"The results are of significant importance since, unlike the current treatments offered for fibromyalgia patients, HBOT is not aiming for just symptomatic improvement," said Efrati. "HBOT is aiming for the actual cause -- the brain pathology responsible for the syndrome. It means that brain repair, including even neuronal regeneration, is possible even for chronic, long-lasting pain syndromes, and we can and should aim for that in any future treatment development."
John Quintner is not convinced.
"I have thought long and hard about this issue and have come to the conclusion that we have been dealing with a 'symptom cluster' rather than with a syndrome," he said. "According to my understanding, fibromyalgia is best explained as an 'idiom of human distress' and, as such, is outside the purview of the biomedical model."