Study Finds Vagus Nerve Stimulation Delays Pain Signals
/By Pat Anson, PNN Editor
Neuromodulation devices that stimulate a key nerve in the neck – the vagus nerve --- have shown potential in treating a variety of chronic pain conditions, including migraines and autoimmune diseases. A new study helps us understand how the devices work.
Researchers studying post-traumatic stress disorder (PTSD) found that vagus nerve stimulation appears to dampen and delay how the brain responds to pain signals.
"It's thought that people with certain differences in how their bodies -- their autonomic and sympathetic nervous systems -- process pain may be more susceptible to PTSD," said Imanuel Lerman, MD, a pain management specialist and associate professor at the University of California San Diego School of Medicine. “And so we wanted to know if we might be able to re-write this 'misfiring' as a means to manage pain, especially for people with PTSD."
UC SAN DIEGO HEALTH
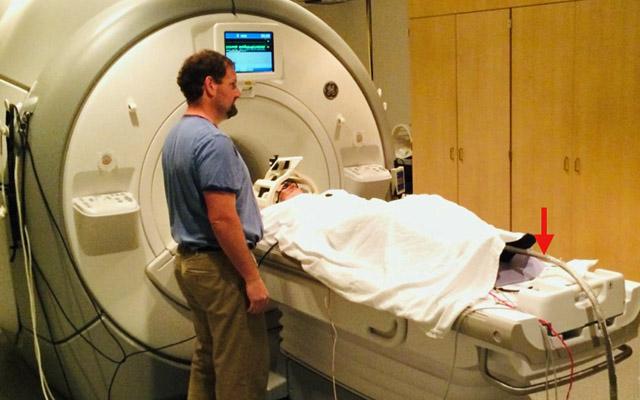
Lerman and his colleagues at Veterans Affairs San Diego Healthcare System used functional magnetic resonance imaging (fMRI) to get a look at the brains of 30 healthy volunteers after a painful heat stimulus was applied to their legs.
Half were treated with vagus nerve stimulation (VNS) for two minutes -- via electrodes placed on the neck – before the heat stimulus. The other half received a mock stimulation.
Researchers found that VNS delayed the response to heat stimulus in several areas of the brain known to be important for sensory and emotional pain processing. These pain-related brain regions were activated ten seconds later than participants who received sham stimulation. Volunteers who received VNS also sweated less in response to the heat.
“Not everyone is the same -- some people may need more vagus nerve stimulation than others to achieve the same outcomes and the necessary frequencies might change over time -- so we'll need to personalize this approach," said Lerman, who reported his findings in the journal PLOS ONE. "But we are hopeful and looking forward to the next steps in moving this approach toward the clinic."
The next step for researchers is to conduct a clinical study of VNS on military veterans in the San Diego area. They want to determine if at-home vagus nerve stimulation can reduce emotional pain and neural inflammation associated with PTSD. People with PTSD often have intrusive memories, negative thoughts, anxiety and chronic pain. It is usually treated with psychotherapy, anti-depressants and anti-anxiety medications.
The Food and Drug Administration has approved VNS for the treatment of pain caused by cluster headache and migraine. A handheld device – called gammaCore – is currently available by prescription for $600 to treat those conditions.
The Feinstein Institute for Medical Research recently reported that VNS significantly reduced pain and fatigue associated with lupus, an autoimmune disease that damages joints, skin and internal organs. In a small pilot study, lupus patients who were treated with VNS for five minutes daily had a significant decrease in pain and fatigue after just five days.
An implanted vagus nerve stimulator is also being tested for the treatment of rheumatoid arthritis.