Why Ice Cream May Be Bad for Your Gut Health
/By David Hilzenrath, KFF Health News
It’s a marvel of food technology: ice cream that resists melting. In a video explaining the science behind it, a seller of food chemicals shows scoops of ice cream holding their shape under hot lights. The super ingredient? Polysorbate 80.
Polysorbate 80 is an emulsifier, a chemical used to control the consistency of thousands of supermarket products. Other widely used emulsifiers or stabilizers include carboxymethyl cellulose, carrageenan, and maltodextrin.
Recently, such ingredients have been showing up in scientific studies for another reason: Researchers say they may cause a variety of health problems.
Studies have found that emulsifiers can alter the mix of bacteria in the gut, known as the microbiome or microbiota; damage the lining of the gastrointestinal tract; and trigger inflammation, potentially contributing to problems elsewhere in the body.
Emulsifiers and stabilizers are among the most common ingredients in ultra-processed foods, a prime target of the “Make America Healthy Again” campaign by Health and Human Services Secretary Robert F. Kennedy Jr.
They are on the department’s radar: Their potentially harmful effects were flagged in a document HHS recently produced to support Kennedy’s drive to eliminate petroleum-based food dyes. But they illustrate the complexity of the war on food additives.
They show how, when it comes to food science, regulators are chronically playing catch-up. In the meantime, for many ingredients, regulators and consumers alike are left in a gray zone between suspicion and proof of harm in humans.
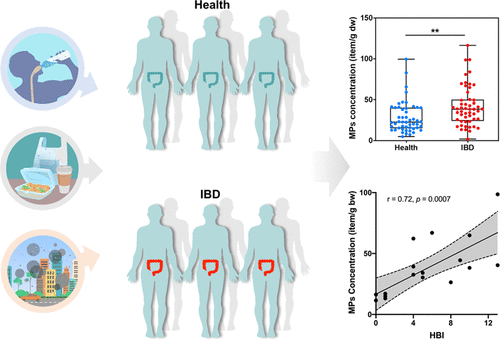
Emulsifiers’ assault on the microbiome could help explain inflammatory bowel diseases such as Crohn’s disease and ulcerative colitis, metabolic disorders, and even cancer, the studies suggest.
“There is a lot of data showing that those compounds are really detrimental for the microbiota and that we should stop using them,” said Benoit Chassaing, a research director at the French National Institute of Health and Medical Research and a co-author of several related studies.
Yet much larger and more ambitious clinical trials in humans are needed, Chassaing added.
For Lewis Rands, who has suffered from gastrointestinal illness, the research fits his own experience as a consumer. Changing his diet to avoid emulsifiers has made a shocking difference, easing symptoms that were debilitating, Rands said.
“Clinically, many patients have reported an improvement in symptoms with such changes,” said Ashwin Ananthakrishnan, a gastroenterologist and researcher at Massachusetts General Hospital.
The scientific findings come with caveats. For instance, much of the research has been done in mice, or by mimicking the human gut in a tube. There are many unknowns. Not all emulsifiers have bad effects, or the same effects, and some people are thought to be much more vulnerable than others.
Even some researchers who have co-authored papers say that the substances have not been proven harmful to humans and that it’s too soon to say regulators should ban them.
Still, the research poses a challenge for the FDA. When emulsifiers began spreading through the food supply, the agency wasn’t focusing on the gut microbiome, a relatively recent scientific frontier, researchers said.
Martin Makary, appointed by President Donald Trump to head the FDA, mentioned the microbiome at his Senate confirmation hearing in March. Though he didn’t cite emulsifiers specifically or identify chemicals by name, he said substances that affect the microbiome deserve the FDA’s attention.
“There’s a body of research now that suggests concern with some of these ingredients,” Makary said. “We have to look at those ingredients, and you have my commitment to do so if confirmed as FDA commissioner.
“These chemicals are creating an inflammatory response in the gastrointestinal tract, and with an altered microbiome lining that GI tract, kids feel sick.”
The FDA and the Department of Health and Human Services did not respond to questions about Makary’s testimony.
However, when journalist Emily Kopp asked HHS for the science behind its recent announcement that it is phasing out petroleum-based food dyes, the agency provided a compilation of information on potentially harmful compounds commonly found in ultraprocessed foods. The document, which appeared to be a draft, included a section on emulsifiers, such as xanthan gum and carrageenan. It noted that the section needed more work.
HHS subsequently provided the document to KFF Health News.
As far back as 2020, an international organization for the study of inflammatory bowel diseases advised that, for people with those conditions, it “may be prudent to limit intake” of maltodextrin, carrageenan, carboxymethyl cellulose, and polysorbate 80.
Emulsifiers are developed from a variety of sources, including plants and bacteria. Some ingredients that might affect the microbiome show up in foods because they were deemed “generally recognized as safe,” or GRAS.
“New information may at any time require reconsideration of the GRAS status of a food ingredient,” the Code of Federal Regulations says.
Ben & Jerry’s vs Häagen-Dazs
Rands, a genetic scientist, took matters into his own hands to battle severe inflammatory bowel disease. The illness caused bloating, stomach pain, cramps, frequent bowel movements, and bleeding, he said.
It left him in a constant state of anxiety and stress, he added, wondering where the nearest bathroom was and whether he’d reach it in time. Even taking a walk around the block with his wife and baby near their home in Australia was problematic.
Then, on the advice of a dietitian, Rands began avoiding foods with emulsifiers: chemicals such as carboxymethyl cellulose, carrageenan, guar gum, xanthan gum, and maltodextrin — plus other additives.
For instance, instead of eating Ben & Jerry’s ice cream, he switched to Häagen-Dazs ice cream that is free of the substances at issue. The relief was dramatic.
“It’s a huge difference,” Rands said. “To me, it’s made more of a difference than any drug.”
He has been able to scale back or stop taking several drugs, which is an added relief — not least because some can have harmful side effects, and, he said, one was taking its toll.
Rands said he used a scientific approach, isolating variables in his diet and logging the results. Avoiding artificial sweeteners helps, he said, but most of the benefit relates to avoiding the emulsifiers.
Ben & Jerry’s did not respond to a request for comment.
‘Science That Hasn’t Been Done Yet’
The Consumer Brands Association, which represents makers of processed foods, stands behind use of the chemicals.
“Food safety and protecting the integrity of the food supply is priority number one for the makers of America’s food and beverage products,” Sarah Gallo, the group’s senior vice president of product policy, said in a statement. “Emulsifiers and thickening agents play an important role in improving food texture and consistency, and have been studied by the FDA through a rigorous scientific and risk-based process.”
Asked for specifics on how the FDA had analyzed potential effects on the microbiome, the group did not respond.
Chassaing said the chemicals were “never considered for the potential effect on the microbiota.”
Robert Califf, who led the FDA under Presidents Barack Obama and Joe Biden, said in an interview that scientists are just beginning to understand the microbiome. He compared it to where the field of genomics was 20 years ago, only much more complicated — “multiplied by a thousand dimensions.”
He said the substances “fell within the standards” when they were greenlighted. “But hopefully most people agree that the standards need to be upgraded,” he added.
“This is different than traditional food safety thinking about, ‘Does it cause an immediate problem?’” Califf said. “We’re talking about long-term health outcomes here.”
And has the FDA evaluated those?
“How could it? There was no way to do it,” Califf said. The answers will vary depending on the emulsifier, and “proving whether it’s bad or good is going to require rigorous science that hasn’t been done yet.”
More recent scientific capabilities expand the possibilities, he said.
‘A Lot of Confusion in the Field’
For a consumer, trying to steer clear of emulsifiers can be difficult. Without realizing it, people can consume a variety of emulsifiers from a variety of foods — and the same chemicals from multiple sources.
Polysorbate 80 was listed as an ingredient on the labels of 2,311 products as of May 12, according to an online database posted by the Environmental Working Group using information from NielsenIQ. Carrageenan was listed on 8,100 product labels; maltodextrin, 12,769; and xanthan gum, 17,153.
Some emulsifiers have multiple names, making them harder to recognize. Some names can apply to more than one emulsifier. And some chemical names that appear on product labels don’t appear in the FDA’s “Substances Added to Food” inventory.
Carboxymethyl cellulose — not to be confused with methyl cellulose — is also known as carboxymethylcellulose and cellulose gum. Maltodextrin can be derived from substances such as cornstarch, rice starch, and wheat starch — but the FDA doesn’t consider it synonymous with the term “modified food starch.”
The naming practices can frustrate efforts to track the chemicals in food, to measure how much of the stuff people are taking in, and even to figure out precisely which chemicals a scientific study evaluated, researchers said.
“There’s a lot of confusion in the field,” said Christine McDonald, a researcher at the Cleveland Clinic who has studied maltodextrin. She called for more consistent naming of additives in the United States.
The very term “emulsifier” is problematic. By strict definition, emulsifiers create an emulsion — a stable blend of liquids that would not otherwise mix, such as oil and water. However, the term is used broadly, encompassing chemicals such as maltodextrin that thicken, stabilize, or alter texture.
Gummed Up
Emulsifiers can be found in foods marketed as natural or healthy as well as ones that look artificial. Some products contain multiple emulsifiers.
Products sold at Whole Foods, for instance, list a variety of emulsifiers on their labels. 365 brand Organic Vegan Ranch Dressing & Dip contained organic tapioca maltodextrin and xanthan gum.
Pacific Seafood Starfish brand Cornmeal Crusted Fishsticks — marked as wild-caught and MSC-certified (sustainably sourced) — contain guar gum. Flour tortillas by 365 included monoglycerides of fatty acids and “stabilizer (guar gum, xanthan gum, carrageenan).”
At a Safeway supermarket, Healthy Choice Grilled Chicken Pesto With Vegetables listed modified potato starch, modified corn starch, carrageenan, xanthan gum, and guar gum.
The label on Newman’s Own Caesar salad dressing said the product contained no artificial preservatives or flavors, no colors from an artificial source, and was gluten-free. The ingredient label listed, “as a thickener,” xanthan gum.
In response to questions for this article, Whole Foods Market said it prohibits more than 300 ingredients commonly found in food.
“Our experts evaluate ingredients for acceptability in all food products we sell based on the best available scientific research,” the company said in a statement provided by spokesperson Rachel Malish.
Safeway’s parent company, Albertsons Companies, did not respond to inquiries. Nor did Pacific Seafood, Newman’s Own, or Conagra Brands, which makes Healthy Choice.
A Growing Body of Research
Research on emulsifiers has been building in recent years.
For example, a study published in January by the Journal of Crohn’s and Colitis concluded that a diet low in emulsifiers is an effective treatment for mild or moderate Crohn’s disease. The eight-week clinical trial, which tracked 154 patients in the United Kingdom, focused on carrageenan, carboxymethyl cellulose, and polysorbate 80.
A study published in February 2024 in the journal PLOS Medicine found that higher intakes of carrageenan and mono- and diglycerides of fatty acids were associated with higher risks of cancer. The study observed 92,000 French adults for an average of 6.7 years.
A study published in September 2023 in The BMJ, formerly known as the British Medical Journal, found that intake of several types of emulsifiers was associated with the risk of cardiovascular disease. The study observed more than 95,000 French adults for a median of 7.4 years.
A series of earlier studies found that emulsifiers “can promote chronic intestinal inflammation in mice”; that two in particular, carboxymethyl cellulose and polysorbate 80, “profoundly impact intestinal microbiota in a manner that promotes gut inflammation and associated disease states”; and that, based on a laboratory study of human samples, “numerous, but not all, commonly used emulsifiers can directly alter gut microbiota in a manner expected to promote intestinal inflammation,” as recounted in a 2021 paper in the journal Microbiome.
Other findings diverge. A study from Australia, published in February in Alimentary Pharmacology and Therapeutics, followed 24 Crohn’s patients over four weeks and concluded that, in the context of a healthy diet, the emulsifier content had “no influence over disease activity.”
The authors declared conflicts of interest, including payments from PepsiCo, drug companies, and Mindset Health Pty, which promotes hypnosis-based therapy. One of the authors, gastroenterology professor Peter Gibson of Monash University in Australia, said the conflicts of interest “have nothing whatsoever to do with the study.”
“It is important not to overinterpret results of studies,” he said, adding that his team’s report “does not mean that emulsifiers are good for you or that there are no health benefits in avoiding emulsifiers.”
Häagen-Dazs ‘Keeps It Real’
Häagen-Dazs touts the absence of such chemicals as a virtue. “Keeping it real, the way it should be,” it said in an online plug for its vanilla ice cream. “No emulsifiers. No stabilizers.”
However, at the company that makes Häagen-Dazs in the United States, Dreyer’s Grand Ice Cream, there are limits to that approach.
Under other brand names — such as Edy’s, Dreyer’s, and Drumstick — it markets products that contain emulsifiers or stabilizers. The company did not respond to questions. In addition, a spokesperson for Nestlé, which markets Drumstick and Häagen-Dazs brands internationally, did not respond.
Drumstick Vanilla Caramel Sundae Cones have no artificial flavors or colors, the package says — but they feature an array of other ingredients, including soy lecithin, guar gum, monogylcerides, and carob bean gum.
The cones, the company’s website says, offer “one incredibly creamy experience.”
But the creamy filling doesn’t melt. Instead, over 24 hours on a KFF Health News reporter’s kitchen counter, it bled a caramel-tinged fluid and shrank into a sticky white foam that could be cut with a knife.
KFF Health News is a national newsroom that produces in-depth journalism about health issues.