Chronic Pain Surged in U.S. After Pandemic
/By Pat Anson
Rates of chronic pain and disabling pain surged in the United States after the Covid pandemic, reaching the highest levels ever recorded, according to a new study.
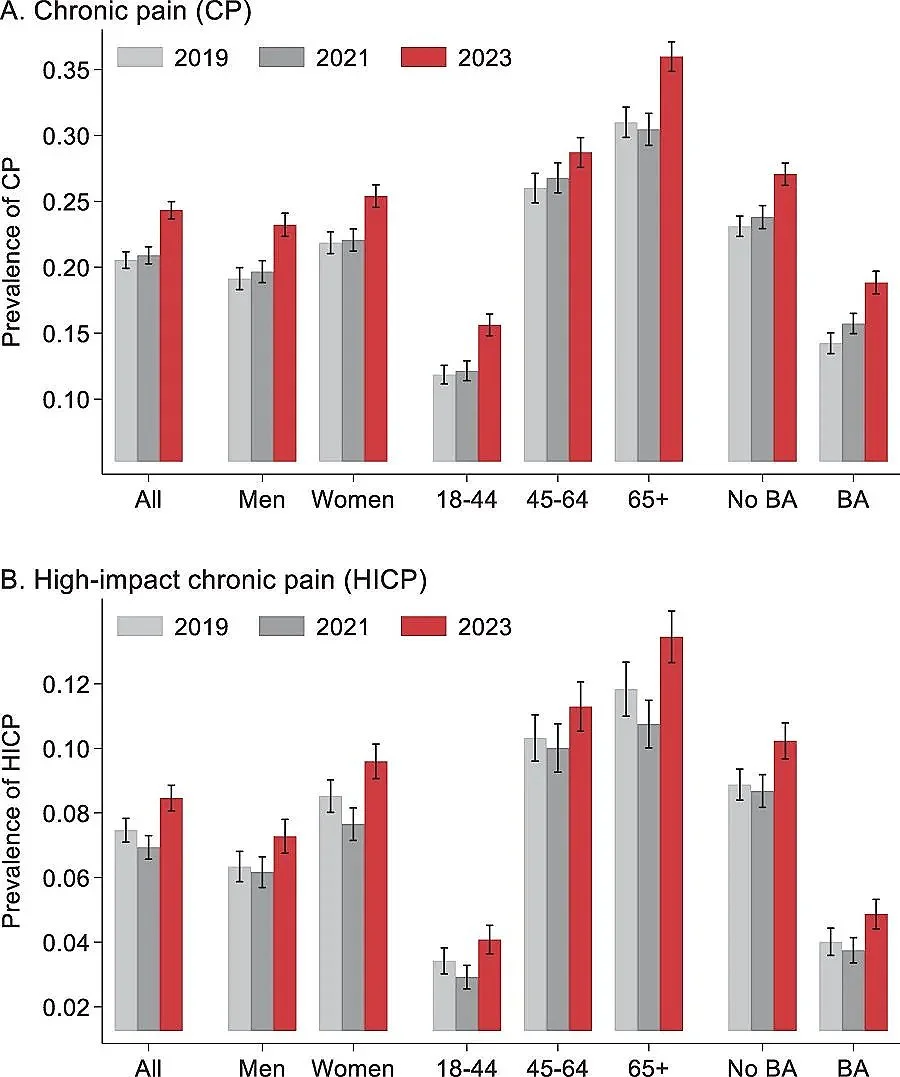
In 2019, about 20.5% of Americans (50 million people) had chronic pain and 7.5% had high-impact pain, which is pain strong enough to limit daily life and work activity.
Pain prevalence remained stable during the pandemic, and by some measures even declined, but in 2023 the chronic pain rate surged to 24.3% of Americans, while high-impact pain rose to 8.9% of the population.
That brought the total number of people who have chronic pain to 60 million, with 21 million having high-impact pain.
“We found that chronic pain, already a widespread health problem, reached an all-time high prevalence in the post-pandemic era, necessitating urgent attention and interventions to address and alleviate this growing health crisis,” wrote co-authors Anna Zajacova, PhD, at Western University in Ontario and Hanna Grol-Prokopczyk, PhD, at the University of Buffalo..
The study is based on results from the 2019, 2021 and 2023 National Health Interview Surveys (NHIS), a federal survey conducted every two years. A preprint of the study was released last year and has now been published in the peer-reviewed journal PAIN.
The 2023 surge in pain was observed in all age, gender, racial/ethnic groups, education levels, and in both rural and urban areas.
Pain increased in almost all body areas, including the back and neck; arms, shoulders and hands; hip, knees and feet; headache or migraine; and in the abdominal, pelvic, and genital areas. The lone area where pain declined was in the jaw or teeth.
Why did pain increase after the pandemic, but not during the pandemic — when people saw doctors less often and postponed or cancelled many health procedures?
One possible explanation is that Covid relief payments, expanded unemployment benefits, and eviction moratoriums eased financial stress.
Working from home and commuting less also lessened physical demands, while giving remote workers more opportunities for self-care.
PAIN journal
“The big question is why we saw this substantial increase in pain prevalence after the pandemic. We examined the role of long COVID and found that it explained about 13% of the increase,” said Grol-Prokopczyk. “None of the other measures we examined — including changes in income or physical health conditions — explained the increase.
“We speculate that abrupt termination of pandemic-era policies, such as remote work arrangements and expanded unemployment benefits, may have played a role.”
In addition to long Covid, researchers also noted an uptick in rates of health conditions that can cause pain, such as arthritis, cancer, cardiovascular disease, diabetes, depression, and anxiety.
The finding of an increase in pain rates conflicts with an FDA analysis that predicted the “medical need” for hydrocodone, oxycodone and other pain relieving Schedule II opioids would decline by 5.3% in 2023. The FDA also predicted a 7.4% decline in the medical use of opioids in 2024 and a 6.6% decline in 2025.
Those FDA projections are important because they are used by the DEA to establish annual production quotas for opioids, which have fallen for nine consecutive years. Since 2015, the DEA has reduced the supply of oxycodone by 68% and hydrocodone by 73%.
When short-term, acute pain is poorly treated, it can have long-term consequences for patients who may transition to chronic pain. Healthcare visits for non–Covid health issues declined dramatically in 2020 and 2021, particularly at hospitals and emergency departments, which are often the first site of care for acute pain management.
Researchers say the lack of adequate and timely pain management during the pandemic may have contributed to more people having chronic pain and high-impact pain in 2023.
“These findings highlight the importance of expanded epidemiological and clinical research on chronic pain to better understand population-level drivers of pain, and to improve national pain prevention and treatment efforts for the many Americans at risk of or affected by pain,” said Grol-Prokopczyk.