Fentanyl Blamed for Half of Massachusetts Overdoses
/By Pat Anson, Editor
New studies in Massachusetts and Rhode Island show that the nation’s fentanyl problem may be much worse than previously thought, while the abuse of opioid pain medication may not be as bad as it is often portrayed.
The Massachusetts Department of Public Health released new data showing that over half of the opioid overdose deaths in the state in 2015 were related to fentanyl, a powerful synthetic opioid that is more potent and dangerous that heroin.
It was the first time toxicology tests were used to detect the presence of fentanyl, a method that is far more accurate than the death certificate codes that the Centers for Disease Control and Prevention uses to classify opioid-related deaths.
“The first-time inclusion of data on fentanyl allows us to have a more honest and transparent analysis of the rising trend of opioid-related deaths that have inundated the Commonwealth in recent years,” said Secretary of Health and Human Services Marylou Sudders.
Of the 1,319 opioid overdose deaths in Massachusetts for which a blood test was available, over 57 percent had a positive result for fentanyl.
The state’s findings do not distinguish between prescription fentanyl that is used to treat more severe forms of chronic pain and illicit fentanyl sold by drug dealers. But it seems likely the vast majority of deaths involve the latter.
illicit fentanyl powder
Massachusetts also released new data from its prescription drug monitoring program for the first quarter of 2016, showing that relativity few pain patients prescribed a Schedule II opioid medication had signs of abusing the drugs. Schedule II opioids include hydrocodone products such as Vicodin and Lortab.
Of the nearly 350,000 patients who had an opioid prescription, the state identified only 484 people (or 0.0014%) as “individuals with activity of concern.” The method used to identify possible abuse was someone receiving Schedule II opioid prescriptions from 4 or more providers and having them filled at 4 or more pharmacies during a three month period.
Rhode Island Overdoses
Rhode Island this week also released a report showing a "significant increase" in fentanyl-related overdoses. Blood tests detected fentanyl in about 60 percent of the state's overdose deaths in the last two and a half months. There have been 28 fentanyl-related overdoses in Rhode Island so far this year.
“People are injecting, swallowing, and snorting this drug without realizing that they are often breathing their last breaths. Unfortunately, fentanyl kills, and it kills quickly,” said Nicole Alexander-Scott, MD, Director of the Rhode Island Department of Health.
Deaths linked to prescription opioids have been in decline in Rhode island for several years. The prescribing of Schedule II and Schedule III drugs in the state has fallen by over a third since 2011.
"The shifts in prescription and illicit drug overdose deaths also began roughly when more focused efforts were undertaken nationally to reduce the supply of prescription drugs," the health department said in a statement.
source: rhode island department of health
‘Alarming’ Rise in Fentanyl Overdoses
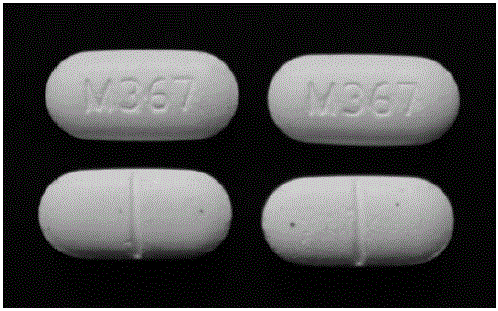
In recent years Rhode Island, Massachusetts and other eastern states have seen a surge in the illicit fentanyl drug trade. The white powdered drug is usually mixed with heroin or cocaine to boost their potency, but in recent months counterfeit pain medication made with fentanyl has appeared on both coasts. The “death pills” are blamed for at least 14 deaths in California and 9 in Florida.
COUNTERFEIT NORCO PILLS
“The counterfeit pills are a newer thing that is going on and that is popping up in different places. It’s certainly something we’re keeping an eye on,” said Erin Artigiani, deputy director of the Center for Substance Abuse Research (CESAR) at the University of Maryland.
CESAR tracks emerging trends in illegal drug use through a nationwide network of more than 1,500 researchers and volunteers.
“It’s very alarming. It’s something we’re very concerned about. And it’s something that local researchers and other members of the network are worried about as well,” Artigiani said.
The appearance of fake pain medication came just as the CDC finalized guidelines that discourage primary care physicians from prescribing opioids for chronic pain. Artigiani stopped short of saying there’s a connection, but admits some pain patients may be seeking opioids on the streets.
“There are people that are looking for other sources or maybe got cutoff by their doctor or maybe their doctor had second thoughts about prescribing pain medications for one reason or another,” said Artigiani. “The people making and selling these illegal drugs are meeting market demand. So if there’s an increase in people looking for pills, then they’re going to make something to sell to those people.”
‘Biased’ CDC Reports
Pain News Network asked to interview someone at CDC about the Massachusetts fentanyl deaths and was told no one would be available.
“We aren’t able to provide comment on non-CDC research,” a spokesperson said in an email. “At CDC we don’t publish state drug overdose death rates for Rx opioids (or for any specific drug type) due to variability in states reporting drugs involved with deaths.”
While CDC may not consider the state data all that reliable, it has not hesitated to use reports from local medical examiners and death certificates in its reports on opioid overdose deaths.
The agency’s most recent report on 2014 overdoses said the U.S. was experiencing an “epidemic of drug overdose” that it blamed largely on prescription opioids.
“Natural and semisynthetic opioids, which include the most commonly prescribed opioid pain relievers, oxycodone and hydrocodone, continue to be involved in more overdose deaths than any other opioid type,” the report states.
Only briefly does the report acknowledge the “emerging and troubling” number of deaths related to illicit fentanyl. Like Massachusetts, CDC cannot distinguish between illicit fentanyl and prescription fentanyl, an important point because all fentanyl related overdoses are classified by the agency as prescription opioid deaths.
The CDC also admits some opioid-related deaths may be counted twice in its reports and some heroin-related deaths may have been misclassified as prescription opioid overdoses.
“We already know that the CDC's info is biased. Not because they are bad people, but because of the way that data is reported to them. Garbage in, garbage out,” says Terri Lewis, PhD, a rehabilitation specialist, medical researcher and patient advocate.
“There is so much variability in the collection of data at the state level, along with the fact that data collection and reporting is voluntary, not mandatory, that one simply cannot rely on the data set. Of course they won't tell you that.”
The CDC uses data on death certificates known as International Classification of Disease (ICD) codes, which do not determine the cause of death, only the conditions that exist at the time of death. Someone could die from lung cancer, for example, but because they were on opioids to relieve cancer pain, an ICD code box for opioids may be checked by a doctor or coroner. Autopsies and toxicology tests are not usually conducted to verify ICD coding.
“The largest part of the problem of reported death certificates is that of variability – local jurisdictions have wide variation in the preparation of individuals who complete these reports, and few are actually physicians or medical examiners. Often local coroners are appointed or elected,” said Lewis. “Until every state is doing exactly the same thing, we have muddy statistics.
“Massachusetts has enacted one of the most sweeping changes to their reporting systems in the country – for that they are to be commended. Distinguishing drugs by the manner of their death is important information for policy managers.”
Until other states and CDC follow Massachusetts’ lead, we may never know the extent of the fentanyl problem. The CDC’s reliance on ICD codes not only distorts the true nature of the nation’s drug problem, but can lead to the misallocation of resources aimed at combating it..
The Obama administration recently asked Congress for an additional $1.1 billion to fight opioid abuse. Most of the money is earmarked for addiction treatment for prescription opioids, not for getting fentanyl off the streets.