AMA: Patients Being Harmed by Rx Opioid Crackdown
/By Pat Anson, PNN Editor
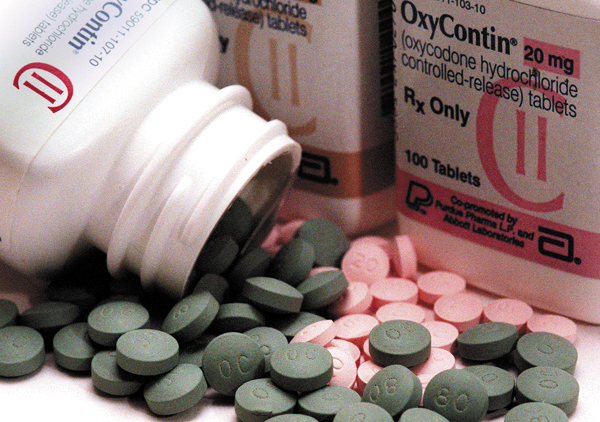
Patients are being harmed by the crackdown on opioid pain medication and increasingly “burdensome” requirements for prior authorization, according to the president of the American Medical Association.
“The pendulum swung too far when pain was designated a vital sign, and now we are in danger of it swinging back so far that patients are being harmed. We need to use our expertise in patient care to change the dialogue to appropriate pain control,” said Barbara McAneny, MD, at a weekend meeting of the AMA.
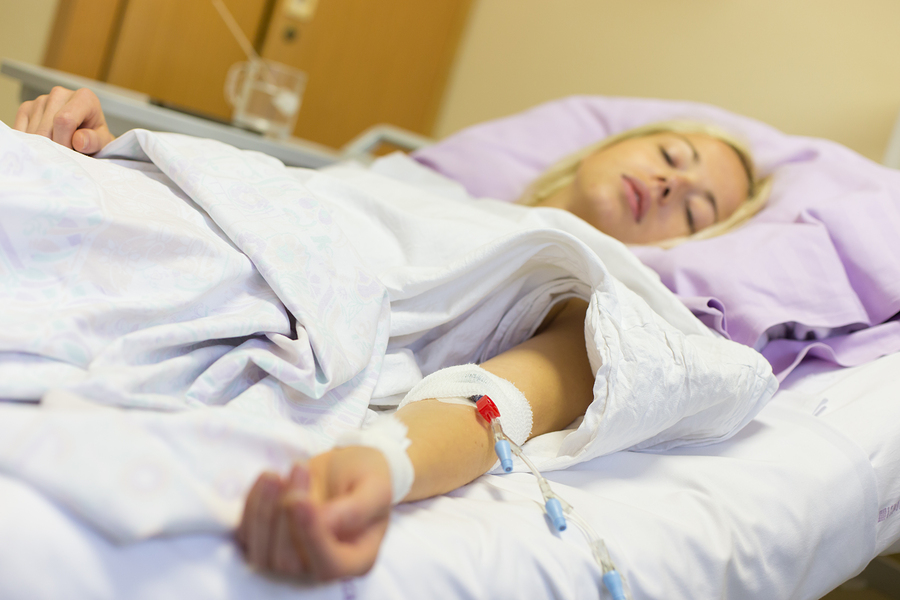
McAneny, who is a practicing oncologist in Gallup, New Mexico, shared the story of a patient with advanced prostate cancer who was in severe pain.
“Metastatic prostate cancer in your bones hurts, and one day he called me to say that his pain regimen wasn’t holding him. So, I increased the dosage of his opioids from two per day to three and of course he ran out early,” McAneny said. “So, I called his primary care physician who agreed to write a prescription for his very large amount of time-release morphine.”
When the patient tried to get his prescription filled, the pharmacist called the insurer for prior authorization and was denied. The pharmacist also checked the prescription drug monitoring program (PDMP) and found that the patient had multiple prescriptions written by McAneny and other doctors.
BARBARA MCANENY, MD (AMA PHOTO)
“The pharmacist suspected my patient was a drug seeker and did not alert me that his prescription was denied. My patient, a very proud man, felt shamed and didn’t know what to do. So, he went home to be as tough as he felt he could be. That worked for about three days and then he tried to kill himself,” said McAneny.
“Fortunately, his family found him in time, and the emergency medicine physician was able to save his life. He spent a week in the hospital and finally we got his pain back under control, on the exact regimen I had prescribed him as an outpatient.”
Ironically, the insurer paid for the patient’s ambulance and hospital bills without any prior authorization. And the CDC’s “voluntary” opioid guidelines — which have been widely adopted by insurers — don’t even apply to cancer patients.
“Like you, I share the nation’s concern that more than 100 people a day die of an overdose. But my patient nearly died of an under-dose. This story illustrates the problems we all confront every day in our current dysfunctional health care system,” McAneny said. “The health plan does not have the chart, doesn’t know the patient, and basically countermanded my orders without even telling me using the prior authorization process. How have we let health plans determine the course of care? They call this quality?
“My patient suffered, in part, because of the crackdown on opioids… When I visited my patient in the hospital as he was recovering from his suicide attempt, I apologized for not knowing his medication was denied. I felt I had failed him.”
McAneny cited a 2017 AMA survey, which found over 90% of doctors believed prior authorization led to delays in treatment and had a negative impact on patient outcomes. Nearly a third of doctors had to wait at least 3 business days for a prior authorization decision to be made.
New prior authorization rules to be adopted by Medicare on January 1 could lead to delays in treatment for millions of elderly and disabled pain patients on high doses of opioids. Prescriptions over 200mg MME (morphine equivalent daily doses) will trigger a “hard edit” safety alert requiring pharmacists to consult with the prescribing physician before filling a prescription. Insurers will also be given greater authority to identify beneficiaries at high risk of addiction and to require they use “only selected prescribers or pharmacies.”