Scrambler Therapy Helped My Daughter Walk Again
/By Reggie Greening, Guest Columnist
Beginning in August 2017, my daughter Amanda began having severe pain in her left foot after spraining her ankle. She was 20 years old at the time and described the pain as feeling as though her bones were being crushed by a red-hot anvil.
Over the next few months, Amanda started having more and more symptoms. It began with sharp pain, then discoloration, and severe swelling set in. This was about the time when she stopped being able to walk and had to be put on opioid medication in an attempt to manage the pain.
The bone crushing sensation began around the end of September, followed closely by burning pain. Amanda was still unable to walk and was taking opioids every four to six hours like clockwork. No one could figure out what was wrong or how to manage the pain other than with opioids.
While attempting to get a diagnosis, Amanda went through many rounds of testing. She had multiple x-rays, two MRIs (one with contrast dye injected intravenously), a three-phase bone scan, a nerve conductivity test, and two phases of bloodwork examined. She also went to a plethora of doctors, including a podiatrist, orthopedist, rheumatologist, dermatologist, physical therapists, homeopathic physician, chiropractor, pain management doctor, and a general medicine doctor.
The podiatrist and one of her physical therapists suspected Complex Regional Pain Syndrome (CRPS), and her podiatrist was the one who eventually determined the diagnosis of CRPS on February 16, 2018.
This spurred my research to find a more sustainable treatment option for Amanda. I spent hours searching online before discovering Scrambler Therapy.
I found a physician in New Jersey who posted videos on YouTube about Scrambler Therapy (also known as Calmare Pain Relief Therapy) and its benefits for those suffering with CRPS and other chronic nerve conditions.
We live in Louisiana, so I looked for a doctor who had a Scrambler Therapy machine closer to our home state. I eventually found a doctor in Dallas who has a machine in his office.
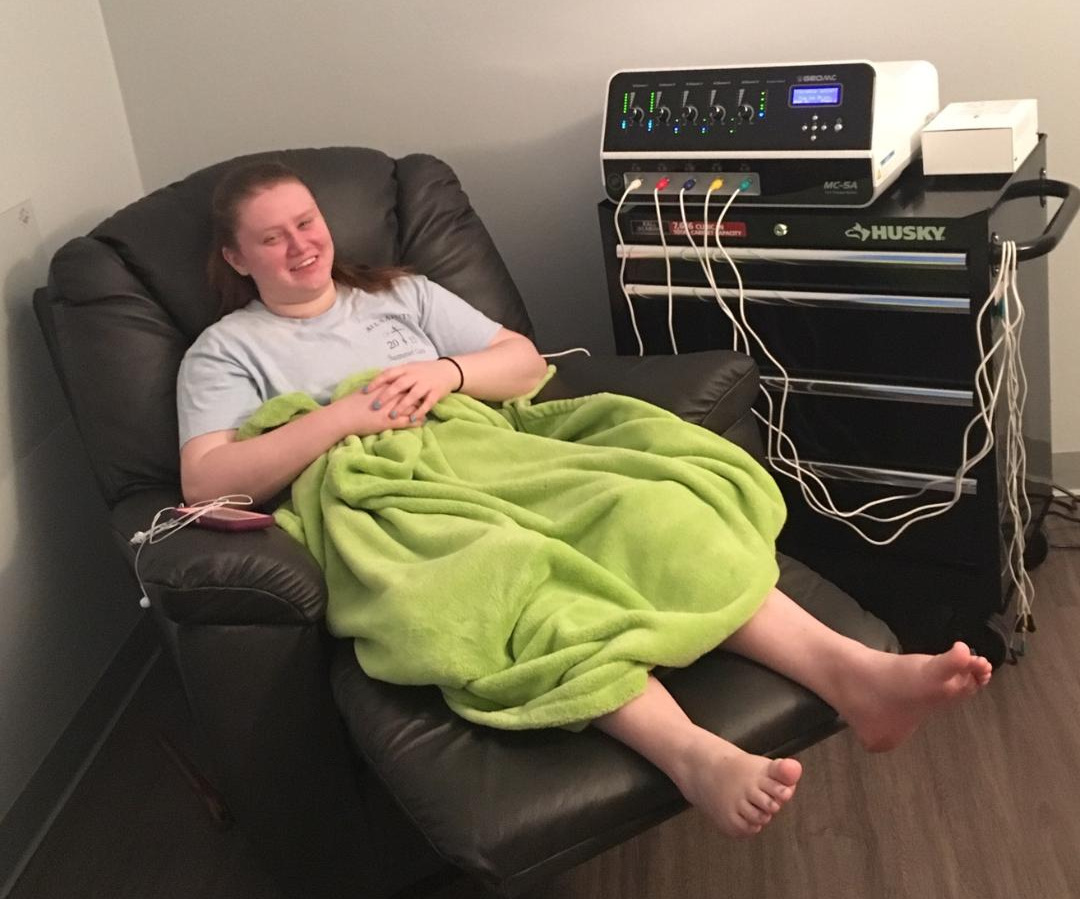
Amanda’s first round of treatment was administered by an osteopathic doctor in March 2018. After the fourth consecutive day of treatment, she was able to walk with the aid of crutches for the first time in seven months. The next day, after her fifth treatment, Amanda was able to walk independently. By the end of her initial round of treatment, she was entirely off opioids and NSAID pain relievers.
Our local TV station did a story about Amanda’s recovery.
Right now, the Scrambler treatment is not covered by insurance and payment for it adds up rather quickly. I am trying to get this therapy more widely acknowledged and known about so that it may become an option for others suffering with chronic neuropathic pain.
I have seen the benefits of Scrambler Therapy firsthand in my daughter. At the time of this writing, Amanda has been off opioids for two months and has been able to maintain the benefits of the initial treatment through booster treatments as needed.
Scrambler Therapy has the potential to help not just those suffering from CRPS (for whom pain relief often seems distant and hopeless), but also for those suffering from other neuropathic pain conditions.
The Greening family lives in Shreveport, Louisiana.
Pain News Network invites other readers to share their stories with us. Send them to editor@painnewsnetwork.org.
The information in this column should not be considered as professional medical advice, diagnosis or treatment. It is for informational purposes only and represents the author’s opinions alone. It does not inherently express or reflect the views, opinions and/or positions of Pain News Network.