Doctors Increasingly Mention Kratom in Patient Notes
/By Crystal Lindell
Kratom is a hot topic these days, as states and local governments scramble to enact bans on the sale of kratom or put age limits on who can purchase the controversial herbal supplement.
Kratom is also being talked about more in hospital settings, according to a new study published in JAMA Network Open.
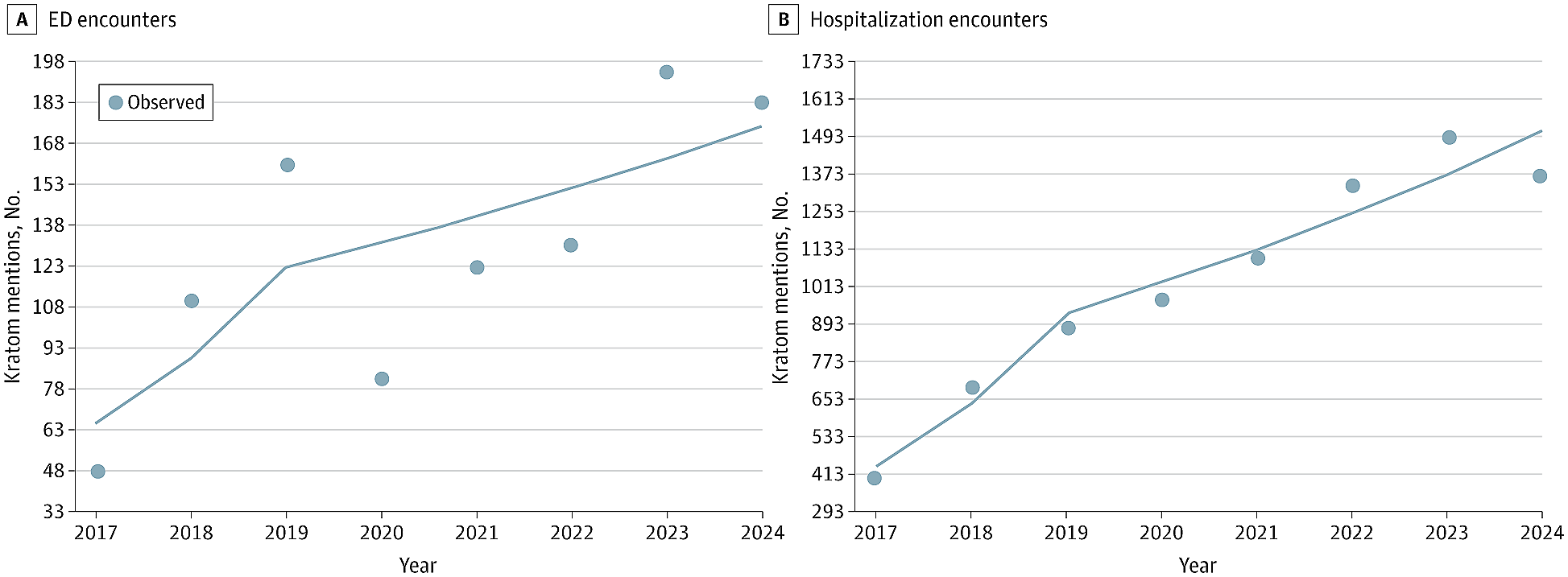
The study looked at how often the word “kratom” was mentioned in clinical notes after an emergency department visit or hospitalization at Mass General Brigham (MGB), a large healthcare system based in Massachusetts.
Researchers looked at patient records between 2017 and 2024, and found a steady increase in kratom being mentioned, both in the ER and in the hospital – about 15% a year in the case of hospitalizations.
Mentions of “Kratom” in Patient Notes
JAMA NETWORK OPEN
Researchers did not analyze the context under which kratom was mentioned, only that that word “kratom” was included in the clinical notes. Whether or not kratom caused a health problem for patients was not studied.
But that didn’t stop researchers from sounding the alarm about the growing use of kratom and its potent alkaloid, 7-hydroxymitragynine (7-OH).
“Clinicians should routinely inquire about kratom use and inform patients of its risks and benefits. While additional research on kratom’s therapeutic potential may be warranted, a focus on the serious adverse effect profile from kratom, 7-hydroxymitragynine, and other kratom alkaloids is urgently needed,” wrote lead author Anika Kopczynski, a clinical researcher at Brigham and Women’s Hospital..
Researchers found that doctors who mentioned kratom in their patient notes were mostly treating white males between the ages of 20 and 49.
Kratom has been used for centuries in Southeast Asia as a natural stimulant and pain reliever, but its use in the United States is relatively new. Estimates on the number of Americans who have used kratom vary widely, from 1.7 million to as many as 20 million.
“The significant increase of encounters with kratom mentioned in our health care system indicates a need for greater clinical awareness,” said Kopczynski.
Kratom has not been approved by the FDA for any medical condition, and health officials say it has opioid-like effects that can lead to addiction and overdoses. The evidence supporting those claims is thin however, as most of the overdoses involve other substances.
While “greater clinical awareness” of kratom and 7-OH is probably a good idea, it’s unclear what advice healthcare providers should give to patients about kratom’s “risks and benefits.”
Should they tell them kratom is “gas station heroin” – as it is often depicted in the media?
Or should they say it is “safe and well tolerated” with “no evidence of meaningful abuse potential,” as a recent study found?
The gap between those two conclusions is likely to confuse both patients and doctors, and lead to less discussion, not more.
Unfortunately, opioid-phobia has turned many patient-doctor appointments into something closer to a visit with a probation officer. And the last thing you want to tell your probation officer about is additional substance use.
Pain sufferers are rightly worried that anything they say will be used against them, and cited as a reason to reduce or even eliminate opioid prescriptions. Even non-opioid patients have a right to be worried about discussing kratom, because they won’t know how that information will be perceived or used.
So it’s a little short-sighted to advise clinicians to ask patients about their kratom use, without also noting how uncomfortable patients may be with that line of questioning.
While I have long called for more research into kratom, the predictable focus on its “serious adverse effect profile” is frustrating. I would argue that research into kratom’s potential benefits is needed just as urgently.
Clearly there’s a need for more education about kratom for medical professionals, but my hope is that some of that education is based on research into actual patient experiences.